- Home
- Migraine Types
- Chronic Migraines
Chronic Migraines: Symptoms, Causes and Long-Term Treatment
Chronic migraines occur when migraine attacks become frequent enough to affect daily life. Doctors diagnose chronic migraine when headaches occur on 15 or more days per month, with at least 8 days meeting migraine criteria.
This chronic condition is one of the most disabling forms of migraine disease. While many people experience occasional migraine attacks, those living with chronic migraine face headaches and neurological symptoms on many days of the month.
Despite the enormous impact chronic migraines have on work, relationships, and quality of life, the condition is still widely misunderstood. Migraine is often dismissed as “just a headache,” when in reality it is a complex neurological disorder that can significantly alter daily life.
 Chronic migraines involve frequent attacks and neurological symptoms that can significantly affect daily life
Chronic migraines involve frequent attacks and neurological symptoms that can significantly affect daily lifeAs awareness of migraine disease grows, more people are finally receiving proper diagnosis and treatment. But for many migraine sufferers, the journey to understanding chronic migraine is still long and frustrating.
What Is a Chronic Migraine?
Doctors diagnose chronic migraine based on the frequency of headache days each month.
According to the diagnostic criteria from the International Headache Society and the International Classification of Headache Disorders, chronic migraine is defined as:
- 15 or more headache days per month
- for at least three months
- with 8 or more days meeting migraine criteria
Migraine symptoms often include:
- throbbing or pulsating pain
- moderate to severe head pain
- pain aggravated by physical activity
- nausea or vomiting
- sensitivity to light, sound, or smell
Chronic migraine is a subtype of migraine disease and often requires preventive treatment strategies, not just medications used during an attack.
Diagnostic Criteria for Chronic Migraine
Chronic migraine is diagnosed using criteria established by the International Headache Society in the International Classification of Headache Disorders.
According to these guidelines, chronic migraine is diagnosed when:
- headaches occur 15 or more days per month
- this pattern continues for at least three months
- 8 or more headache days per month meet migraine criteria
- the headaches are not better explained by another headache disorder
Migraine headache days typically include symptoms such as:
- throbbing or pulsating pain
- moderate to severe intensity
- pain that worsens with physical activity
- nausea or vomiting
- sensitivity to light or sound
These diagnostic criteria help doctors distinguish chronic migraine from other headache disorders such as tension-type headache or medication overuse headache.
If migraine attacks occur frequently, a healthcare provider may recommend preventive treatment strategies to reduce attack frequency and improve quality of life.
Episodic Migraine vs Chronic Migraine
Many people begin with episodic migraine, where attacks occur occasionally but not frequently enough to be classified as chronic.
Doctors distinguish the two based on how often headaches occur.
Episodic migraine
- Fewer than 15 headache days per month
- Migraine attacks occur periodically
- Symptoms may still be severe but occur less frequently
Chronic migraine
- 15 or more headache days per month
- At least 8 migraine days per month
- This pattern continues for more than three months
Some people move between episodic and chronic migraine over time. When migraine attacks gradually increase in frequency, the process is sometimes called migraine chronification.
Early treatment, trigger management, and preventive strategies may help reduce the risk of migraine becoming chronic.
Doctors often describe the transition from episodic migraine to chronic migraine as migraine chronification, where attacks gradually become more frequent over time.
Why Migraines Become Chronic
Many people begin with episodic migraine, where attacks occur occasionally. Over time, however, migraine attacks may become more frequent until they meet the criteria for chronic migraine.
This process is sometimes called migraine chronification, where the brain gradually becomes more sensitive to migraine triggers and neurological stimulation.
Researchers believe several factors can increase the risk of migraine becoming chronic.
Frequent Untreated Migraine Attacks
When migraine attacks are not treated early or effectively, the nervous system may remain in a heightened state of sensitivity. Repeated attacks can make the brain more reactive to pain signals and triggers.
This is one reason neurologists emphasize treating migraine attacks early when symptoms first appear.
Medication Overuse
Ironically, medications used to relieve migraine pain can sometimes contribute to more frequent headaches when used too often.
This condition is known as medication overuse headache (MOH). It may occur when pain medications or triptans are used very frequently over long periods.
Managing medication use carefully with the help of a healthcare provider can reduce this risk.
Stress and Lifestyle Factors
Chronic stress, poor sleep patterns, irregular meals, and dehydration can all contribute to increased migraine frequency.
When these factors occur repeatedly, the nervous system may become more sensitive to migraine triggers.
Hormonal Changes
Hormonal fluctuations can also play a role in migraine frequency, particularly for women. Changes in estrogen levels during menstrual cycles, pregnancy, or menopause may influence migraine patterns.
Genetic Susceptibility
Migraine has a strong genetic component. Some individuals are simply more vulnerable to developing chronic migraine because of inherited neurological differences.
Researchers continue to study the genetic mechanisms involved in migraine disease to develop more targeted treatments.
The Importance of Early Management
While not all migraine progression can be prevented, early management of migraine attacks and triggers may reduce the likelihood of migraine becoming chronic.
Strategies that may help include:
- identifying and managing triggers
- using preventive treatments when appropriate
- maintaining consistent sleep and hydration patterns
- working with a healthcare professional to develop an effective migraine treatment plan
Understanding how migraine patterns evolve over time can help people take proactive steps to protect their long-term neurological health.
Learn more about migraine symptoms and early warning signs.
Signs Your Migraines May Be Becoming Chronic
Sometimes migraine attacks gradually become more frequent without people realizing the change right away.
Some warning signs that migraine patterns may be shifting toward chronic migraine include:
- headaches occurring more than once a week
- needing medication for headaches more frequently
- shorter recovery time between migraine attacks
- increasing sensitivity to light, sound, or smell
- fatigue or brain fog between attacks
If migraine attacks begin occurring on many days of the month, it is important to discuss this pattern with a healthcare provider. Early treatment adjustments can sometimes help prevent migraine frequency from increasing further.
Tracking migraine symptoms and triggers can help you recognize when migraine patterns are changing. → See my symptom and trigger trackers
Why Chronic Migraines Are Often Misunderstood
The disability caused by chronic migraine is frequently underestimated by society, healthcare systems, and even some medical professionals.
The World Health Organization has repeatedly ranked migraine among the leading causes of disability worldwide.
Research estimates that:
- 15–18% of women experience migraine
- 6–8% of men experience migraine
- around 2% of children are affected
Yet migraine disease continues to be underdiagnosed and undertreated in many parts of the world.
One reason is stigma. Migraine is still too often described as a simple headache that should be ignored or pushed through, when in reality it is a neurological disorder involving complex changes in brain signaling and nerve sensitivity.
 Chronic migraines are a neurological disorder causing frequent migraine attacks and disability
Chronic migraines are a neurological disorder causing frequent migraine attacks and disabilityHow Chronic Migraines Affect Daily Life
Living with chronic migraine means dealing with symptoms that can affect nearly every part of life.
Migraine attacks may involve much more than head pain. Many people experience:
- extreme fatigue
- cognitive difficulties or “brain fog”
Over time, the unpredictability of these symptoms can make it difficult to maintain regular work schedules, social commitments, or daily routines.
The financial impact can also be significant, as medical costs increase while work productivity may decrease.
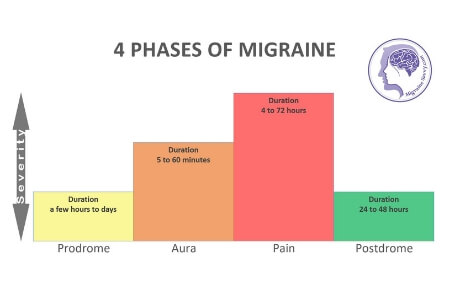
Chronic migraine often develops gradually as migraine attacks become more frequent. If you want to understand how migraine symptoms develop throughout the different stages of an attack, see my article on The 4 Stages of Migraine.
My First Migraine Attack: A Personal Experience
I remember my first migraine attack clearly.
I was 32 years old and working in Sydney when it hit without warning. I had just eaten a chocolate bar during a break when, about half an hour later, intense nausea and severe pain suddenly appeared on the right side of my head.
Within minutes I was vomiting and struggling to see clearly from one eye. By the time I reached the ferry to go home, I could barely stay upright.
At the time I had no idea what was happening.
Looking back now, I realize that moment marked the beginning of a long journey with migraine disease — one that would eventually become chronic.
Over the years my migraine patterns have changed many times. Some attacks start in my neck, others behind my eyes. Sometimes they bring emotional swings, other times overwhelming fatigue.
Migraine is rarely predictable.
Learn Directly from Leading Migraine Specialists
Living with migraine can feel overwhelming, especially when treatments don’t work the way you hoped or when people around you don’t understand the condition.
If you are struggling with frequent migraine attacks, learning directly from experienced neurologists and headache specialists can provide valuable insight into what may help.
Each year, the Migraine World Summit features interviews with leading migraine neurologists, researchers, and patient advocates to discuss the latest developments in migraine science and treatment.
During the event, experts share practical information about:
- migraine prevention strategies
- treatment advances and medications
- lifestyle and trigger management
- emerging migraine research
- ways to improve quality of life with migraine
The summit streams free online for one week each year, allowing you to watch the interviews from home.
If you prefer to watch the sessions at your own pace, lifetime access is also available.
→ See the migraine experts speaking this year
How to Prevent Chronic Migraines
Preventing chronic migraine usually requires a combination of medical treatment and lifestyle strategies.
Doctors often recommend preventive treatments when migraine attacks occur frequently.
These may include:
Some supplements, regular exercise, and consistent sleep routines may also help reduce migraine frequency for some individuals.
Because chronic migraine affects the entire nervous system, many people benefit from addressing both physical and emotional health when developing a treatment plan.
Managing the Emotional Impact of Chronic Migraine
Living with chronic migraine can be emotionally exhausting. Depression and anxiety are common comorbid conditions associated with migraine disease.
Talking with a healthcare professional, therapist, or support group can make a meaningful difference when coping with the long-term effects of chronic illness.
For many people, practices such as journaling, meditation, or gratitude exercises can help shift focus toward resilience and emotional balance during difficult periods.
Migraine may slow life down, but it can also provide opportunities to reassess priorities and focus on what truly matters.
Getting the Right Support
If migraine attacks are becoming more frequent or interfering with daily life, it is important to seek professional medical advice.
A healthcare provider can help determine whether migraine has become chronic and recommend appropriate treatment strategies.
Learning to recognize your symptoms early and taking action quickly can make a significant difference in managing migraine attacks over time.
Ready to take the next step?
Choose the next step that fits where you are right now.