- Home
- Migraine Types
- 7 Tips For Coping With Silent Migraine
7 Tips For Coping With Silent Migraine
I could not believe that someone could have a silent migraine, a migraine without pain. A painless migraine! I instantly thought of a friend who just gets lightning bolts in the right side of his vision for 4 hours, and then it goes away. That's it - no pain. But others feel paralyzed, how scary is that!
Below are 7 tips to help you cope with silent attacks.
My #1 Choice in Magnesium Supplementation
I get intense pain and that pain phase is the most recognized phase of a classic migraine.
Silent, painless migraines miss the pain phase but still go through all the other phases.
It can have an aura, or not! Visual disturbances are most typically the first of the symptoms.
Experts also refer to this condition as migraine aura without headache. They are also called: acephalgic migraine, optical migraine, visual migraine, painless migraine and ocular migraine.
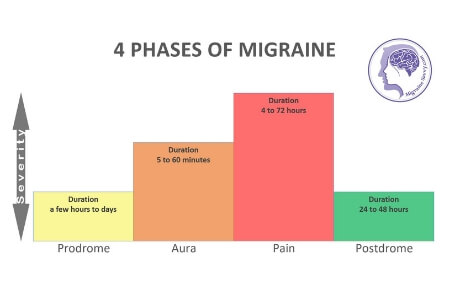
As I already mentioned, this migraine type attack still has the symptoms and phases of a classic migraine attack but it just misses the pain phase. Let me briefly explain the four phases of classic migraine so you can have a better understanding before we get to the tips:
Phase #1 - Prodrome – the “prodrome” phase is your early warning signal that a migraine is on its way. Symptoms can be experienced a day or two before the actual attack but only 1 out of every 4 sufferers get a prodrome. Symptoms look like: irritability, confusion, extreme yawning and thirst, tiredness and diarrhea. Symptoms vary between attacks and individuals.
Phase #2 - Aura – the aura is most typically associated with the visual disturbances of an attack. Like the zig zag lines or blotted out sections in your central vision. But aura can also encompass the disruption of motor and language functions. 1 in 5 sufferers experience an aura before the pain phase. Most of the research says that aura can last for about an hour, but mine can last for 2 days before an attack. So again, aura symptoms can vary.
Phase #3 – Pain – the pain phase is the most recognized phase in migraines. This is the phase that silent migraine misses. The headache pain is normally one sided and can be accompanied by nausea and vomiting. Extreme over sensitivity to light, noise and movement are also in this phase. This phase can last from a few hours to, most commonly, 72 hours.
Phase #4 – Postdrome – this phase can also last for 24 hours or so after a migraine attack. Silent migraine sufferers also experience this phase. The symptoms look like fatigue and melancholy or light depression.
You may feel the need to sleep it all off. In fact, sleep may be the only treatment you need.
So individuals who suffer with silent, painless migraines experience all of the other three phases along with their own unique pattern of symptoms.
For more details on the 4 phases of migraine and silent symptoms, please click on complex migraines and silent migraine symptoms.
My #1 Choice in Magnesium Supplements
9 Out of 10 Migraineurs Can Not Function Normally
Individuals that experience silent painless migraines still experience symptoms severe enough to need bed rest. Even without the disabling pain phase, the other symptoms interfere with normal functioning. Many experience visual symptoms so intense that they feel like they are hallucinating.
The infamous Lewis Caroll who wrote Alice in Wonderland is suspected to have been a migraine sufferer who experienced feeling huge and tiny and hallucinated quite vividly during his attacks.
Cortical spreading depression still occurs with these attacks, reducing brain activity. This wave has been confirmed by functional MRI technology when mapping out how the brain is affected during an attack. The visual field is almost always affected. For more specific details please read the post on what are migraines.
The Same Triggers
Silent attacks seem to have the same triggers as classical migraine attacks. These include: foods like chocolate, red wine, aged cheeses, fermented and pickled foods; stress; lack of sleep; alcohol; weather; tyramine; hormones; loud noise; and bright flickering lights.
For more details on triggers, please read our articles on common migraine triggers and foods that trigger migraines.
7 Tips to Help You Cope With Your Silent Migraine Headache Attacks
The unique pattern of silent migraine symptoms have puzzled Doctors and scientists alike. The answer is still elusive in the mystery of migraine.
Here are seven tips to help you cope with your challenging silent migraine headache attacks:
1. Keep a migraine diary. Keep track of your symptoms. When they start and when they end. Download this symptom tracker to help with this. Keep a list of your food and drinks, changes in your sleeping routine or stress levels, and any other things that might be a potential trigger.
2. Make a list of what you're already taking. Make a list of all the prescription and over-the-counter medications you are taking to avoid any problems with drug interactions. Make a list of supplements too. You can also make a list of things you have taken that did not work to stop your silent migraine attack.
3. See your doctor. Take your diary with you so your doctor has more detailed information about you and what might be going on. S/he will be the one to diagnose silent migraine for you. In most cases they will test to rule out more serious medical problems, like a stroke or brain tumor.
4. Request to see a Neurologist who specializes in silent migraine. If your doctor does not give you a referral, then ask for one. Ask for someone who specializes in your exact migraine type diagnosis.
5. Consider all treatment options. Medications are the first line of treatment from your doctor. There are numerous medications, over 100 in fact, used to treat migraine attacks according to the Migraine Research Foundation. I find triptans are the best drugs available to date (for me).
Be prepared for some trial and error before you find the right one for you. You may also want to consider preventative medications as well, depending on how often your episodes occur.
6. Avoid your known triggers. This one almost goes without saying. Most migraineurs know to avoid what triggers them into scary zone! If you have not got that far yet, feel free to read the article on avoiding your migraine triggers.
7. Consider some new lifestyle changes. Don't underestimate the power of this one. Do what you can to be proactive and prevent your next attack. Things like: eating regularly, eating nutritious foods, having a regular sleep routine, exercising regularly and learning some stress management techniques will work wonders to reduce and ease your migraine symptoms.
My #1 Choice in Magnesium Supplements
Ready to take the next step?
Choose the next step that fits where you are right now.
MIGRAINE TYPES Related Articles
Reference:
1. Lava, Neil MD (2015) What are Silent Migraines? Available [Online] at: https://www.webmd.com/migraines-headaches/what-are-silent-migraines#1 Accessed Jul 4, 2016 Updated Mar. 9, 2019