- Home
- Migraine Symptoms
- Can a Migraine Cause Vertigo
Can a Migraine Cause Vertigo? Symptoms, Causes and What You Can Do
Can a migraine cause vertigo?
Yes. And if you are feeling dizzy, off balance, rocking, swaying, or spinning — even without head pain — migraine could absolutely be the reason.
When this happens, it is often called vestibular migraine or migraine associated vertigo. It is one of the most common causes of ongoing unexplained dizziness.
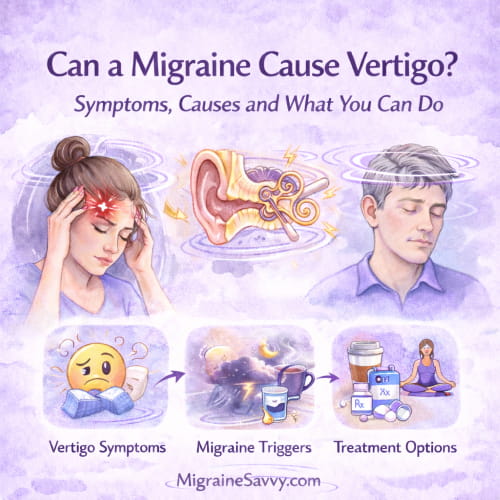 Can a migraine cause vertigo? Yes. Vestibular migraine can trigger dizziness, imbalance, and motion sensitivity even without headache.
Can a migraine cause vertigo? Yes. Vestibular migraine can trigger dizziness, imbalance, and motion sensitivity even without headache.If you have been told your scans are normal, your ears are fine, and “maybe it’s anxiety,” I want you to know something.
You are not imagining it.
Let me walk you through this clearly.
What Is Migraine Associated Vertigo?
Migraine associated vertigo, now more commonly called vestibular migraine, is a neurological condition that affects your balance system.
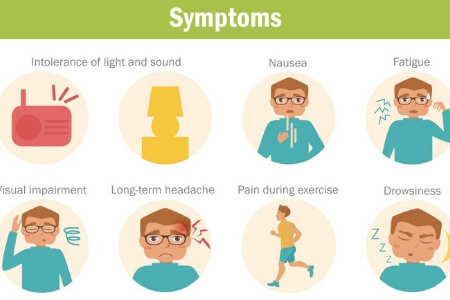
It can feel like:
- Spinning (true vertigo)
- Rocking or swaying when you are still
- Feeling pulled to one side
- Motion sensitivity
- Nausea
- Light sensitivity
- Brain fog
- Ear fullness or ringing
And here is what makes it confusing.
You may not have a headache at all.
That is why many people are misdiagnosed with Ménière’s disease, vestibular neuritis, or even panic disorder before someone finally connects it back to migraine.
Migraine is not just head pain. It is a brain sensitivity disorder. Vertigo is one of the ways that sensitivity can show up.
Can a Migraine Cause Vertigo Without Headache?
Yes. And this is where it gets especially frustrating.
Migraine associated vertigo without headache is common. You might have:
- Severe spinning
- Vomiting
- Motion intolerance
- Days of imbalance
And never experience your “typical” migraine pain.
If you had migraines earlier in life, you are more likely to develop vestibular symptoms later.
So if you are asking yourself again, can a migraine cause vertigo even without pain?
The answer is still yes.
If you want a broader overview of migraine symptoms, read → Migraine Symptoms Explained
What Causes Vestibular Migraine?
The exact mechanism is still being studied, but we understand the basics.
Migraine affects:
- Brainstem pathways
- Sensory processing centers
- The trigeminal nerve
- The vestibular system, which controls balance
When that system becomes hypersensitive, your brain misinterprets movement signals. You feel spinning when nothing is spinning.
Hormones, stress, sleep disruption, dehydration, and certain foods can lower your threshold.
You are not weak.
Your brain is reactive.
There is a difference.
How Is Vestibular Migraine Diagnosed?
If you’re wondering how doctors confirm this, here’s the honest answer.
There is no single test.
Vestibular migraine is diagnosed clinically. That means your doctor listens carefully to your history and symptom pattern.
Typically, diagnosis involves:
- A history of migraine (past or present)
- Recurrent vertigo or dizziness episodes
- Episodes lasting minutes to hours (sometimes days)
- Normal MRI and hearing tests
- No better explanation for the symptoms
Many people go through:
- MRI scans
- Hearing tests
- ENT consultations
- Balance testing
Only to be told everything is “normal.”
That can feel invalidating.
But migraine is a functional neurological condition. It does not show up on scans. The diagnosis comes from pattern recognition.
If your dizziness keeps returning and other causes have been ruled out, migraine should absolutely be considered.
How to Treat Vestibular Migraine
How to treat vestibular migraine depends on frequency and severity.
If episodes are occasional, your doctor may focus on acute treatment.
If they are frequent or constant, preventive therapy is usually needed.
Treatment options may include:
- Triptans
- Gepants
- Anti-nausea medication
- Beta blockers
- Calcium channel blockers
- Topiramate
- Amitriptyline
- CGRP medications in some cases
It may take experimentation to find the right combination. That is normal.
If you are working with the wrong doctor, you may never get the right treatment plan. A neurologist who understands migraine is essential.
You can also read → Headache Doctor Appointments: How to Be More Effective
Vestibular Migraine Treatment at Home
Medication is not the whole picture.
Vestibular migraine treatment at home focuses on stabilizing your nervous system.
That means:
- Consistent sleep
- Regular meals
- Electrolyte hydration
- Stress regulation
- Reducing medication overuse
For some people, magnesium and riboflavin can support prevention.
If stress is a major trigger for you, you may want to explore → Meditation for Migraine Relief
Structure lowers threshold volatility.
When your brain feels safe and predictable, symptoms calm down.
Why Anxiety Often Shows Up With Vestibular Migraine
If you feel anxious when the room spins, that does not mean anxiety caused it.
Vertigo is disorienting. It triggers your survival system.
Your brain senses instability and activates fight-or-flight.
That surge of adrenaline can then:
- Increase nausea
- Increase heart rate
- Increase light sensitivity
- Increase the perception of dizziness
It becomes a loop.
The dizziness creates anxiety. The anxiety amplifies the dizziness.
Breaking that loop matters.
That’s why stress regulation, breathwork, structured routines, and sometimes cognitive behavioral therapy can be powerful additions to medical treatment.
You are not “crazy.”
Your nervous system is reacting to instability.
And it can be retrained.
Physical Therapy for Vestibular Migraine
Physical therapy for vestibular migraine, also called Vestibular Rehabilitation Therapy (VRT), can be life changing.
A trained vestibular physiotherapist helps you:
- Improve gaze stability
- Retrain balance pathways
- Reduce motion sensitivity
- Build walking confidence again
If you feel like you cannot trust your body, this therapy helps rebuild that trust.
It does not cure migraine, but it teaches your brain how to compensate more effectively.
When You Should See a Specialist
If your dizziness is worsening…
If you are vomiting repeatedly…
If medications are not helping…
If you are being told it is “just stress” but you know something is wrong…
Please push for a referral.
You deserve clarity.
And if you are experiencing new neurological symptoms such as weakness, speech difficulty, or sudden severe headache, seek urgent medical evaluation.
Most cases of migraine associated vertigo are not dangerous.
But new symptoms should never be ignored.
Learn Directly from Leading Migraine Specialists
Living with migraine can feel overwhelming, especially when treatments don’t work the way you hoped or when people around you don’t understand the condition.
If you are struggling with frequent migraine attacks, learning directly from experienced neurologists and headache specialists can provide valuable insight into what may help.
Each year, the Migraine World Summit features interviews with leading migraine neurologists, researchers, and patient advocates to discuss the latest developments in migraine science and treatment.
During the event, experts share practical information about:
- migraine prevention strategies
- treatment advances and medications
- lifestyle and trigger management
- emerging migraine research
- ways to improve quality of life with migraine
The summit streams free online for one week each year, allowing you to watch the interviews from home.
If you prefer to watch the sessions at your own pace, lifetime access is also available.
→ See the migraine experts speaking this year
Does Vestibular Migraine Go Away?
Sometimes.
For some people, episodes reduce significantly over time with proper treatment and lifestyle stabilization.
For others, it becomes a long-term condition that needs structured management.
What makes the biggest difference is:
- Early diagnosis
- Avoiding medication overuse
- Consistent preventive care
- Working with the right specialist
When managed properly, most people regain normal function.
Hope is realistic here.
A Practical Next Step
If vertigo is part of your migraine pattern, tracking becomes essential.
- When do symptoms start?
- What were you doing before they began?
- How long do they last?
- What helped?
You can explore structured tracking tools here → Migraine Symptom & Trigger Trackers
When you understand your pattern, fear reduces.
And when fear reduces, symptoms often do too.
Ready to take the next step?
Choose the next step that fits where you are right now.