- Home
- Migraine Education
- Migraine Brain Vs Normal Brain
Migraine Brain vs Normal Brain: How Pain Works in the Migraine Brain
Understanding the difference between the migraine brain vs normal brain helps explain why migraine pain behaves so differently from other types of headaches.
Migraine is not simply a severe headache. It is a neurological condition involving changes in brain signaling, inflammation, and sensory processing. These changes affect how the brain interprets pain, responds to sensory stimuli, and regulates blood vessels.
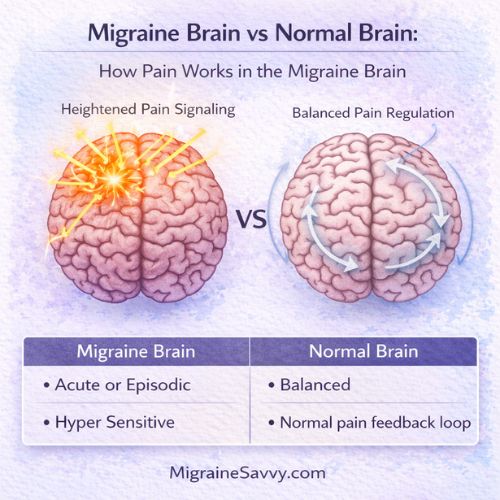 Comparison illustration showing how the migraine brain processes pain differently from a normal brain
Comparison illustration showing how the migraine brain processes pain differently from a normal brain
During the 2020 Migraine World Summit, neurologist Patricia Pozo Rosich, MD, PhD explained how the migraine brain can develop a pain feedback loop that makes attacks more frequent over time.
This article summarizes key insights from that discussion and explains how migraine pain develops, why it can become chronic, and what strategies may help break the cycle.
If you're unsure whether your symptoms are migraine or another type of head pain, read my guide explaining the difference between migraine and headache:
→ Migraine vs Headache: Understanding the Critical Differences
Migraine Brain vs Normal Brain: What’s the Difference?
The main difference between a migraine brain vs normal brain is how pain signals are processed and amplified.
In people with migraine, the brain is more sensitive to sensory input and more likely to activate inflammatory pathways that trigger migraine attacks. This heightened sensitivity means the migraine brain can enter a repeating pain cycle that becomes harder to stop over time.
Researchers believe migraine involves several interacting systems, including:
- nerve signaling pathways
- inflammation in the brain's protective tissues
- blood vessel regulation
- sensory processing networks
Because these systems interact, migraine attacks can involve symptoms far beyond head pain, including nausea, dizziness, fatigue, and sensitivity to light or sound.
How Pain Works in the Migraine Brain
During the Migraine World Summit interview, Dr. Pozo Rosich explained several key differences between normal pain responses and migraine pain cycles.
These insights help explain why migraine can become chronic and why early treatment is important.
Does Pain Provide Any Benefit for Chronic Migraine?
In most situations, pain acts as a warning signal that something is wrong in the body.
However, migraine pain does not function this way.
Migraine attacks are not simply warning signals about injury or illness. Instead, they are the result of neurological processes that activate pain pathways even when no physical damage is occurring.
For people living with chronic migraine, the brain may begin to learn and repeat pain patterns, creating a feedback loop that increases the likelihood of future attacks.
The Difference Between Acute Pain and Chronic Pain
Acute pain normally alerts us to injury or danger. It activates protective responses that help us avoid harm.
Chronic pain behaves differently.
When pain occurs frequently over time, the brain can begin to adapt to the repeated signals. In some cases, the nervous system becomes more sensitive to pain triggers and begins activating pain responses more easily.
Migraine is an example of this type of neurological pain cycle.
Once the cycle becomes established, it can take multiple treatment strategies to interrupt it.
Why Do Some People Experience Pain More Intensely?
Researchers are still exploring why some individuals experience migraine more frequently or more intensely than others.
One factor may involve CGRP (calcitonin gene-related peptide), a molecule known to play a major role in migraine attacks.
Animal studies have shown that when CGRP is introduced into certain areas of the brain's protective covering (the dura), it can trigger pain-like responses.
Interestingly, these responses were stronger in female rats than in male rats, suggesting biological differences that may help explain why migraine occurs more often in women.
Migraine is especially common during the reproductive years, which suggests that hormones may also play a role.
What Brain Changes Occur During Migraine?
Modern brain imaging techniques such as functional MRI (fMRI) allow researchers to observe how different parts of the brain activate during pain.
Although pain itself cannot be seen directly on brain scans, researchers can observe patterns of brain activity associated with migraine attacks.
These scans show that migraine involves activation of multiple brain regions related to:
- pain processing
- emotional response
- sensory input
- motor responses
Some brain changes associated with chronic migraine appear to be dynamic, meaning they can improve when migraine is treated effectively.
However, other changes may persist over time.
This is one reason why early treatment and prevention strategies are so important.
How the Migraine Pain Cycle Forms
Migraine attacks often involve inflammation in the dura, the protective tissue surrounding the brain.
This inflammation can last for several days, which is one reason migraine attacks commonly last between two and three days.
Over time, repeated migraine attacks can lower the brain's threshold for triggering future attacks.
Fear or anticipation of the next migraine can also influence the brain's sensitivity.
In some people, attacks may begin to occur at predictable times of day because the brain has learned to repeat the pattern.
Breaking this cycle early can improve long-term treatment outcomes.
Research suggests that patients with episodic migraine often respond better to preventive treatments than those whose migraines have already become chronic.
Strategies for Managing Chronic Migraine Pain
Managing migraine often requires a combination of strategies rather than a single treatment.
Dr. Pozo Rosich described several important pillars of migraine management.
Education and Understanding
Education plays a critical role in migraine treatment.
Understanding how migraine works can help patients recognize triggers, follow treatment plans more effectively, and reduce anxiety related to attacks.
Learning about migraine can also help people make informed decisions about prevention strategies.
Choosing the Right Medical Treatment
Migraine treatment often involves both preventive medications and acute medications.
Preventive treatments aim to reduce the frequency and severity of attacks, while acute treatments are used to stop attacks once they begin.
Doctors must consider several factors when selecting treatments, including:
- other health conditions
- sleep quality
- mood and anxiety levels
- blood pressure and vascular health
Migraine is considered a neurovascular condition, meaning both nerve signaling and blood vessels are involved.
For this reason, treatment approaches often need to address multiple factors.
Addressing Stress and Triggers
Chronic migraine often develops after periods of intense stress or major life changes.
Identifying these patterns can help people understand why their migraines may have become chronic.
Developing better coping strategies, stress management techniques, and support systems can play an important role in long-term migraine management.
Working with a supportive healthcare provider is also essential. If you feel your doctor is not listening to your concerns, seeking another specialist may be helpful.
Earlier intervention can change the shape of your life.
~ Patricia Pozo Rosich, MD, PhD
Learn Directly from Leading Migraine Specialists
Living with migraine can feel overwhelming, especially when treatments don’t work the way you hoped or when people around you don’t understand the condition.
If you are struggling with frequent migraine attacks, learning directly from experienced neurologists and headache specialists can provide valuable insight into what may help.
Each year, the Migraine World Summit features interviews with leading migraine neurologists, researchers, and patient advocates to discuss the latest developments in migraine science and treatment.
During the event, experts share practical information about:
- migraine prevention strategies
- treatment advances and medications
- lifestyle and trigger management
- emerging migraine research
- ways to improve quality of life with migraine
The summit streams free online for one week each year, allowing you to watch the interviews from home.
If you prefer to watch the sessions at your own pace, lifetime access is also available.
→ See the migraine experts speaking this year
Final Thoughts
The difference between the migraine brain vs normal brain helps explain why migraine attacks behave so differently from typical headaches.
Migraine involves complex neurological processes that affect pain pathways, inflammation, and sensory processing. These changes can create repeating pain cycles that become harder to control over time.
Understanding how migraine works is one of the most powerful steps toward improving treatment and prevention.
With the right education, medical support, and management strategies, many people can significantly reduce the impact migraine has on their lives.
Ready to take the next step?
Choose the next step that fits where you are right now.
MIGRAINE EDUCATION Related Articles
Migraine Brain vs Normal Brain References
1. Migraine World Summit (2020). Interview with Patricia Pozo Rosich, MD, PhD.
2. Pozo Rosich P. (2016). Eight out of ten migraine patients do not use the correct medication. La Vanguardia.